By DR. ELISA MARIA BIANCHI
Each year in the United States about 150,00 new cases of colorectal cancer are diagnosed and approximately 53,000 Americans will die of the disease. Even as the mortality rate for colorectal cancers has been on the decline since 1990, it continues to be the third most common cause of death for both men and women in the United States. In contrast to the overall mortality decline, the incidence in patients under the age of 50 has been steadily increasing since 1992. This represents a chilling trend, especially given the low likelihood that patients under 50 will undergo screening colonoscopy.
Laparoscopic assisted colorectal surgery is widely used in the treatment of this disease. Many colorectal surgeons have adapted laparoscopic surgery as their technique of choice for most of the abdominal procedures they perform. Laparoscopic surgery for the treatment of colorectal cancers is widely used because it does not compromise oncological outcomes and allows for rapid postoperative recovery. However, laparoscopic low pelvic dissections are extremely technically demanding, particularly in male patients who tend to have narrow pelvises. Furthermore, laparoscopic instruments are non-articulating, thus requiring unnatural coordination and non-ergonomic positioning. This is all done with imaging systems that only provide flat, 2-dimensional views. What’s more, laparoscopic low rectal cancer surgery has a high rate of conversion to open surgery and has an increased rate of postoperative male sexual dysfunction. While we have made many advances in the last decades, laparoscopic surgery still has numerous drawbacks.
Robotic surgery is an alternative method of performing minimally invasive colon and rectal surgery. The technology has evolved greatly since it was first used for colon and rectal surgery in 2001. The modern iteration of robotic assisted surgery begins with NASA, developed as an outgrowth of virtual reality systems for visualizing data being returned from the Voyager mission. This idea then developed into telepresence surgery, or remote robotic surgery. First developed as a prototype for use by the military to provide remote immediate surgical care on the battlefield. Eventually, the PUMA 560 system was the first robotic device used to perform robotic assisted surgery, a percutaneous brain biopsy in 1985.
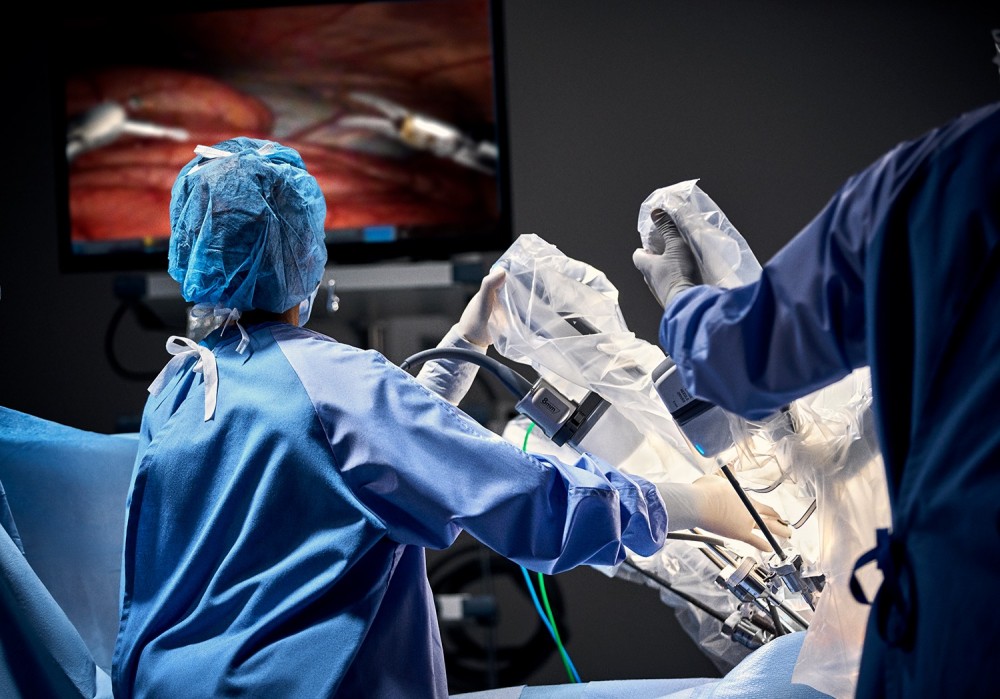
Robotic surgery has evolved over the years and is today largely used by surgeons who are physically in the same room as their patients. In 1999, the da Vinci Robotic Surgical System entered the market. This robotic system was notable for its three-dimensional vision system, three arms and EndoWrist® technology. In 2014 the Xi system was introduced and has fast become the most widely used system. This robotic platform has four arms, allows for multi-quadrant surgery, has upgraded optics and technology that improves arm positioning. Robotic assisted surgery, especially in the pelvis, provides many advantages over laparoscopic techniques. It eliminates many of the technical difficulties inherent to laparoscopic surgery, as its multiple, flexible surgical arms are not limited by lack of articulation or narrow spaces, such as in the male pelvis. It allows for 3-dimentional views, which makes it much easier to identify structures like the inferior hypogastric plexus. Surgeons are also able to directly control the camera and are not dependent on an assistant to “hold the camera steady.” Another advantage of the robotic system is that it allows surgeons to have more ergonomic positioning while operating, which then causes less physical strain and fatigue. All of these factors represent technical improvements over the laparoscopic technique. Therefore, in my practice I favor the use of the robotic system anytime that it is feasible.
Minimally invasive surgery, broadly speaking, has shown advantages for patient’s outcomes, in both the long and short term. However, the lack of complete adoption of minimally invasive techniques in colorectal surgery and other fields may be due to the difficulties associated with laparoscopy. Although robotic surgery technology was initially developed for telepresence surgery, it has evolved as an answer to the technical difficulties that surgeons face with laparoscopic surgery. Robotic colorectal surgery has developed to offer multiple approaches that include hybrid and non-hybrid operations (using the robot exclusively or with hand and/or laparoscopic assistance). There are multiple docking strategies and designs to improve mobilization and dissection. This technique continues to evolve over time and provides safety and flexibility to surgeons as they tackle the treatment of colorectal cancer. These benefits are notable in low rectal cancers and, in particular, with male patients. As a Colorectal Surgeon, I look forward to the improvement and evolution of robotic surgery, including areas such as single port systems and endoscopic robotic surgery. The increased adoption of this technique promises to improve the outcomes for colorectal cancer patients and help stem the tide of colon and rectal cancers.
Elisa Maria Bianchi, MD, is a Board-Certified general surgeon at Digestive and Liver Center of Florida who completed a colorectal surgery fellowship at Zucker School of Medicine at Hofstra/Northwell Health in New York where her specialty training encompassed a variety of small bowel, colon, rectal and anal pathologies which included malignant, benign and inflammatory disease (Crohn’s disease and ulcerative colitis). She previously completed her residency in general surgery at Loma Linda University Health with particular emphasis in robotic techniques.
Bianchi completed her medical training at the University Illinois at Chicago. Prior to that she completed an undergraduate degree in bioengineering at the University of Illinois and worked as an engineer at Abbott Laboratories. Dr. Bianchi is fluent in Spanish. www.dlcfl.com